Under the leadership of the AUGS Board, the Society’s councils are dedicated to advancing the Board approved strategic plan and supporting the future growth of AUGS. This nimble and effective governance structure supports collaboration across committees. Keep reading to learn more about each AUGS Committee’s unique focus. Click on the committee name to view the charter which includes roles, responsibilities, and qualifications.
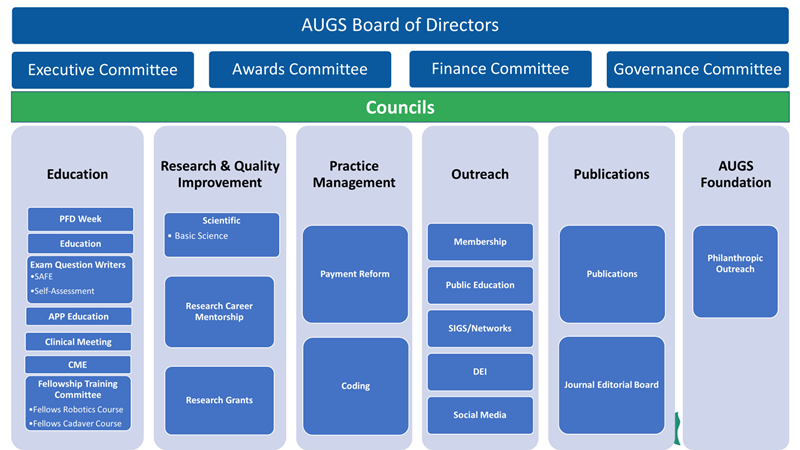
Board Level Committees
Executive Committee
Purpose: The Executive Committee acts on behalf of the Board of Directors in the intervals in between Board meetings only to the extent that it knows how the Board of Directors would act on any given topic. In unusual cases, usually due to the timeliness of decisions, the Executive Committee may act on a matter when the Board’s position is not clear. The Executive Committee also functions as the “personnel committee” of the Board of Directors, performing the annual performance review of the Executive Director, based on the input of the Board of Directors.
Awards Committee
Purpose: The AUGS Awards Committee serves the Society through soliciting and reviewing nominations annually for AUGS awards.
Members: TBD (Chair), Catherine Bradley (Immediate Past President), Emily Lukacz (Vice President), Amy Park (PFD Week Vice Chair), Cary Fishburne (Membership Committee Rep), Karolynn Echols (DEI Committee Rep)
Finance Committee
Purpose: The Finance Committee serves the Society through the oversight of the AUGS and Foundation budget to ensure sound financial practices. Ongoing committee activities include providing review and oversight to the monthly financial reports, investments, and records; and providing guidance on the preparation of the annual budget and annual audit.
Members: Dobie Giles (Chair/Treasurer), Emily Lukacz (Vice President), Heidi Brown (Foundation), Zaid Chaudhry, Geoffrey Towers, Jerome Yaklic
Governance Committee
Purpose: The Governance Committee serves both the Society and Foundation through oversight of the process and governance by which they function. Ongoing activities include review of the policy and procedures manual and bylaws, conducting an annual assessment of the Board of Directors, ensuring conflicts of interest are disclosed and handled appropriately, overseeing the Call for Volunteers and Call for Board Nominations processes including vetting of Board candidates, and reviewing and monitoring best practices in association management.
Members: Tanaz Ferzandi, MD (Chair/President Elect), Emily Lukacz, MD (Vice President), Catherine Bradley, MD (Immediate Past President), Marianna Alperin, MD (Board member), Geoff Cundiff, MD (Past President), Stacey Barnes, AUGS CEO (Ex-Officio member)
Education Council
PFD Week Program Committee
Purpose: The PFD Week Program Committee is charged with maintaining and enhancing PFD Week, AUGS’ annual meeting, to ensure it is the leading meeting for health care professionals interested in urogynecology education. The Committee is charged with developing programming that maximizes the attendee experience and focuses on the latest scientific and surgical advances in the field.
Members: Danielle Antosh (Chair), Amy Park, MD (Vice Chair), Nimota Adeboye, Ijeoma Agu, Lindsay Burnett, Caroline Cox, Catrina Crisp, Gabriela Halder, Joseph Pincus, Lauren Siff, Julie Starr, Elena Tunitsky–Bitton
Education Committee
Purpose: The Education Committee evaluates the educational needs of urogynecologists, gynecologists and urologists focused on urogynecology and reconstructive pelvic surgery and develops an educational strategy which is responsive to those needs.
Members: Christina Lewicky-Gaupp (Chair), Taji Yazdany (Vice Chair), Rob Gutman (Board Liaison), Sarah Ashmore, Katherine Husk, Colin Johnson, Padma Kandadai, Kimia Menhaji, Lauren Rascoff, Lauren Stewart, Mary Duarte Thibault, Christine Vaccaro, Eva Welch
Fellowship Training Committee
Purpose: The Fellows Training Committee evaluates the educational needs of Urogynecology and Reconstructive Pelvic Surgery fellows and fellowship programs and develop programs and services that AUGS can provide. The Fellowship Training Committee oversees the Robotics Course and Fellows Cadaver Course planning committees.
Members: John Occhino (Chair), Leslie Rickey (Vice Chair), Rob Gutman (Board Liaison), Peter Aziz, Lauren Caldwell, Monique Hiersoux Vaughan, Christopher Hong, Joseph Kowalski, Lioudmila Lipetskaia, Hoa Nguyen, Lauren Nicola-Ducey, Nicole Roselli, Elena Tunitsky, Emily Von Bargen
Robotics Course Planning Committee
Purpose: The Robotics Course Planning Committee oversees the development of a one-of-a-kind course, available to fellows, featuring a full day in the robotic lab and one day in didactic sessions.
Fellows Cadaver/Hands On Course Planning Committee
Purpose: The Fellows Cadaver Course Planning Committee oversees the development of an advanced vaginal surgery course for specialist fellows in Urogynecology and Reconstructive Pelvic Surgery and those in Female Urology, already well versed in basic vaginal surgery, who are looking to increase their knowledge about more complex vaginally approached and laparoscopic/robotic operations.
Advanced Practice Provider Course Planning Committee
Purpose: The APP Course Planning Committee evaluates the educational needs of allied health professionals focused on Urogynecology and Reconstructive Pelvic Surgery and develop programs and services that address those needs.
Members: Katie Propst (Vice Chair), Carissa Aboubakare (Vice Chair), Rob Gutman (Board Liaison), Jennider Dillman, Diane Newman, Melania Velasquez
CME Committee
Purpose: The CME committee is charged with ensuring AUGS meets and/or exceeds all requirements for accreditation by the Accreditation Council for Continuing Medical Education (ACCME); reviewing policies and procedures to assure that the educational activities of the Society are developed and offered in a manner consistent with the requirements of the ACCME; and evaluating program quality, needs assessment, review speakers’ content for all CME programs and provide feedback to planning committee chairs on how to improve the scientific content for courses/meetings
Clinical Meeting Planning Committee
Purpose: The Clinical Meeting Planning Committee oversees the development of a course that is clinically focused and assists physicians with staying informed on the latest clinical advancements in the field, as well as how to run a practice in today’s environment.
Members: Miles Murphy (Chair), Roger Goldberg (Vice Chair), Rob Gutman (Board Liaison), Rosa Carbonell, Omar Duenas Garcia, Deborah Karp, Arnulfo Martinez
Question Writing Group
The Question Writing Group oversees the writing, reviewing, scoring and distribution of the annual AUGS Self-Assessment Fellows Exam (SAFE) Exam and the Urogynecology Self-Assessment Exam.
Members: Sallie Oliphant (Chair), Lindsay Turner (Vice Chair), Rob Gutman (Board Liaison), Lauri Budnick, Jenifer Byrnes, Christina Escobar, Katherine Husk, Lioudmila Lipetskaia, Jaime Long, Saya Segal, Stuart Shippey, Ruchira Singh, Geoffrey Towers, Eva Welch, Marcella G Willis-Gray, Vaneesha Vallabh-Patel
Research & Quality Improvement Council
Scientific Committee
Purpose: The Scientific Committee supports the research component of AUGS’ mission by advising and facilitating the advancement of research through funding, education, and advocacy. The Committee focuses on increasing and maintaining the workforce of the urogynecology physician-scientists and researchers to catalyze the advancement of clinical practice with an end goal of improving care through impactful research. Members of the Scientific Committee represent the various research areas within urogynecology and serve as advocates to advance this mission.
Members: Colleen McDermott (Chair), Isuzu Meyer (Vice Chair), Naz Siddiqui (Board Liaison), Marsha Guess (Basic Science Subcommittee Chair), Milena Weinstein (Grants Review Chair), Rachel High, Kimberly Kenne, Edward Kim, Rachel High, Julia Shinnick, David Sheyn, Kenan Song, Amanda White
Basic Science Sub-Committee Members: Marsha Guess (Chair), Robert Kelley (Vice Chair), Amanda Artsen, Lindsay Burnett, Rui Liang, Michael Pezzillo
Purpose: The Academic Career Mentoring Committee serves the Society through the identification and administration of mentorship opportunities for members interested in establishing a career in an academic setting both with and without research interest.
Members: Victoria Handa (Chair), Cecile Ferrando (Vice Chair), Naz Siddiqui (Board Liaison), Mary Ackenbom, Amanda Clark, Cara Grimes
Purpose: The Grants Committee serves the Society through the oversight of the grants program. Goals of the mentored research grant program are to support the pilot projects to help fulfill the AUGS Foundation's mission of supporting novel clinical, translational, and bench research directions and enabling junior investigators to obtain future independent funding for research focused on female pelvic medicine.
Members: Milena Weinstein (Chair), Pamela Moalli (Vice Chair), Naz Siddiqui (Board Liaison), Cynthia Fok, Kristen Gerjevic, Nancy Ringel, Rodger Rothenberger
Practice Management Council
Coding and Reimbursement Committee
Purpose: The Coding and Reimbursement Committee is charged with educating AUGS members on current coding procedures. Ongoing committee activities include addressing payment and coverage issues, answering coding questions from members, developing fact sheets for the AUGS website, and writing coding articles for Urogyn News. The committee also responds to Commercial Carriers and regional MACs when nationally accepted policy is being ignored.
Members: Charles Thompson (Chair), Jameca Price (Vice Chair), Board Liaison: Matt Barker, Rebecca Batladen, Ashley Carroll, Sarah Collins, Yanghee Courbron, Jessica Harroche, Fareesa Kahn, Mamta Mamik, Stephanie Molden, Gnankang Napoe, Mitch Schuster, Nemi Shah, Azin Shahryarinejad, Mitch Schuster (Advisor), Marc Toglia (Advisor), Scott Poehlmann (Advisor)
Payment Reform Committee
Purpose: The Payment Reform Committee serves the Society through gaining expertise in the development and execution of alternative payment models (APM) as defined by CMS and addressing payment reform issues as needed.
Outreach Council
Membership Committee
Purpose: The Membership Committee serves the Society by representing and monitoring the needs of the membership and ensuring a strong membership structure and benefits package. Additional ongoing activities include oversight of member recruitment and retention campaigns, evaluating the needs of membership segments, approval of SIG applications and Life Membership requests, and periodically reviewing existing programs, services and technology platforms to ensure that they enhance the AUGS member experience.
Members: Kurian Thott (Chair), Cary Fishburne (Vice Chair), Jennifer Cera, Samuel Chacon, Deepanjana Das, Betsy Greenleaf, Adam Hare, Amie Kawasaki, James Ross, Budi Iman Santoso, Gazala Siddiqui
Public Education Committee
Purpose: The Public Education Committee is charged with representing and monitoring AUGS’ outreach efforts to the public about the Urogynecology and Reconstructive Pelvic Surgery subspecialty and role of the urogynecologist. The committee ensures the seamless integration of all patient-related programs and services on behalf of AUGS. Ongoing activities includes oversight of the Voice for PFD website, development of patient education materials to be used by patients and physicians, and oversight of medial relations activities.
Members: Renee Bassaly (Chair), Lopa Pandya (Vice Chair), Sana Ansari, Elizabeth Brehman, Christine Chu, Lisa Dabney, Alexandra Dubinskaya, Gena Dunivan, Marcus Ortega, Priyanka Kadam Halani, Sarah Rabice, Anna Romanova, Ladin Yuteri-Kaplan
Special Interest Groups/Community Groups
Purpose: SIGs and Community Groups serve the Society through the creating and fostering community feeling around a designated area of interest that brings together AUGS members for information exchange and sharing.
Diversity, Equity and Inclusion Committee
Purpose: The DEI Committee serves the Society through the creation and identification of opportunities for expanding the conversation regarding diversity, equity, and inclusion within AUGS and amongst its board, committees, and member communities.
Members: Elisa Trowbridge (Chair), Marian Acevedo Alvarez (Vice Chair), Surbhi Agrawal, Sarah Boyd, Charelle Carter-Brooks, Katherine Dengler, Karolynn Echols, Kristin Hung
Social Media Committee
Purpose: The Social Media Committee is charged with assisting staff in the development and execution of strategy for AUGS programs and services, which includes but is not limited to
Urogynecology journal, Voices for PFD, and educational programming. Ongoing committee activities include identifying areas of growth and engagement, monitoring social media trends, developing social media resources for members, and maintaining and implementing a social media strategy.
Members: Ian Fields (Chair), Cassandra Kisby (Vice Chair), Jocelyn Fitzgerald (Social Media Editor), Stephanie Glass Clark, Vinita Gottipati, Jena Hall, Deborah Levy, Shazia Malik, Camelia Malkami, Elizabeth Southworth, Miriam Toaff, Aldene Zeno
Publications Council
Publications Committee
Purpose: The AUGS Publications Committee provides oversight to the development of clinical publications, including Clinical Guidance Documents (ie, Clinical Practice Statements, Clinical Consensus Statements, Terminology Reports, and Systematic Reviews), Research Reports, Advocacy Documents (ie, Position Statements and White Papers), and Practice Advisories. The committee ensures the documents produced by writing groups and other AUGS committees and networks are of high quality, consistent form and content, and accurate terminology to ensure successful publication in
Urogynecology and/or on the AUGS website. Furthermore, the committee represents AUGS in cross society efforts for the development of joint publications as appropriate.
Members: Scott W. Smilen (Chair), Jerry Lowder (Vice Chair), Gina Northington (Board Liaison), Tirsit Asfaw, Megan Bradley, Olivia Cardenas-Trowers, Lauren Cadish, Olivia Chang, Sara B. Cichowski, Angela DiCarlo-Meacham, Autumn Edenfield, Cara L. Grimes, Anne Hardart, Peter Jeppson, Kate V. Meriwether, Emily Whitcomb, William Winkelman
Urogynecology Journal
Purpose: The Journal Editorial Board oversees the publication of Urogynecology, a peer-reviewed, multidisciplinary journal dedicated to specialists, physicians and allied health professionals concerned with prevention, diagnosis and treatment of female pelvic floor disorders. Current Editorial Board Members.
AUGS Foundation
The Philanthropy and Development Committee serves the Society by ensuring that AUGS’ fundraising and development efforts are in concert with the Society's strategic direction and financial needs. The committee serves as the mechanism by which members are involved in the fundraising process.
Members: Kim Ferrante (Chair), Thythy Pham (Vice Chair), Heidi Brown (Board Liaisons), Megan Jasko, Lisa Peacock, Jon Pennycuff, Kristina Warner, Erika Wasenda